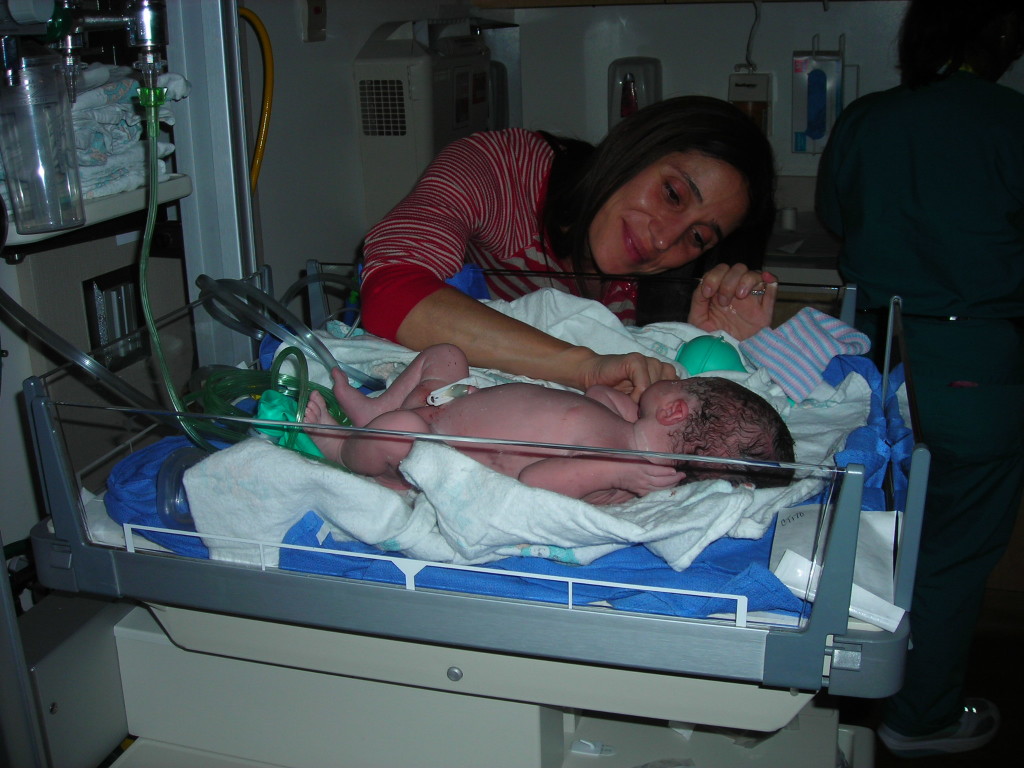
Surrogacy: A Love Story, Part Five
Hello, friends. Here’s the fifth part of our series by writer Kelly Weiss Rogondino, who is generously sharing her personal journey with us. Read on for a powerful and candid look at the effects of cancer and the challenges and rewards of surrogacy.
I haven’t yet mentioned how I fared emotionally during the pregnancy. As a gestational surrogate, Lisa carried an embryo conceived from my egg and my husband’s sperm, therefore the baby is genetically ours with no genetic link to Lisa. Many people don’t know that there is more than one type of surrogate. With a traditional surrogate for a married heterosexual couple, the wife’s eggs are not used (for medical reasons) but the husband’s sperm is used to conceive the embryo, with the surrogate’s eggs. Therefore the husband has a genetic link to the baby, and the wife would have to adopt the baby from the surrogate after he/she is born. This is the type of situation where you hear stories about the surrogate changing her mind and wanting to keep the baby. Even in cases of gestational surrogacy, the surrogate can and to some extent, does, become attached to the fetus. The difference is that there is no genetic link between the fetus and the surrogate with a gestational surrogacy and there is no legal right of the surrogate to claim parentage. Even so, after we were pregnant with our daughter, people would ask me if I was worried that Lisa would run off with our baby. No, I didn’t worry about Lisa running off with our baby. I was more concerned about not experiencing everything that Lisa was and missing out on bonding with my baby in utero and yes, there was the occasional irrational thought. That baby was not growing inside of my body and I felt helpless. Once my eggs were retrieved, I was rendered medically useless.
I had no right to be anything but overjoyed and grateful. I was both of those things, but I was also jealous that Lisa got to carry my baby and feel her moving and I couldn’t. When I was with Lisa and she would caress her belly, I would die inside. I wanted to feel what she was feeling. Every time an ultrasound tech or nurse would address Lisa as if she were the mom (everyone’s presumption), I would want to cry and scream “I am the Mom!” That is MY baby in there! I don’t know if these are normal responses and feelings, but they were my feelings. I wasn’t treated like the mom because I wasn’t carrying the baby. When I called the doctor’s office where the amnio was performed because they had billed Lisa and not me for the procedure, they wouldn’t talk to me because I wasn’t the patient. When I pre-registered Lisa at the hospital (and this is a hospital in Los Angeles that should be used to surrogate deliveries), they repeatedly sent me paperwork with Lisa indicated as the genetic mother. The administrative office of the hospital initially filled out the birth certificate incorrectly, giving my baby Lisa’s last name, even though they had spoken with me many times and had certified copies of the court documents establishing me and my husband as the genetic parents. My husband and I received “visitor” badges when we checked Lisa in to the hospital (Lisa and our daughter, once she was born, had the matching wristbands) and we weren’t allowed to both be in the room with Lisa and another “visitor” (only 2 visitors at a time). If my ob/gyn hadn’t delivered the baby, they probably would have handed her to Lisa first instead of me. After Lisa checked out of the hospital, even though I had pre-paid for her post-delivery room for an additional night so that my husband and I could handle the nighttime feedings and bond with our daughter, they said they needed the room and we couldn’t stay. The hospital’s “patient liaison” for the maternity ward took pity on us and allowed my husband and I to sleep in an employee lounge until our daughter was released.
It took months after my daughter was born to get the bills and paperwork straightened out with the hospital billing office because I wasn’t the patient (though I was the responsible financial party). My insurance company, whom I had spoken to several times before my daughter’s birth, had assured me that she would be added to my policy as soon as she was born as long as I notified them within a few days of birth. I notified them the same day she was born but they initially rejected my daughter’s physician and hospital bills. It was a never ending cycle of incorrect bills, rejected insurance claims, and re-telling my story over and over again to one administrator after another and sometimes even repeating it to the same person more than once. None of this was Lisa’s fault or under her control whatsoever, but it didn’t help my emotional state. I was handling all of these insurance and billing issues on little sleep as even less patience as I was a new mom and had enough to deal with. Finally, after several months, one day I spoke with someone at the hospital who took the time to really understand the situation, put all of the missing pieces in place, and he corrected everything in an afternoon.
Regarding the hospital bill, because Lisa didn’t have medical insurance and because my insurance wouldn’t cover my daughter until after she was born, Lisa was considered a “cash” patient and my husband and I were financially responsible for all of the hospital and delivery costs. If you show up at a hospital to give birth and you have no insurance, the cost of a regular vaginal delivery with no complications starts at about $32,000 (or at least it did in 2009). Starts there. However, if you are lucky enough to be “in the know” about these things (I got a tip from someone at my doctor’s office), you can contact the hospital in advance and enter into a “cash agreement” with them. This means that you pre-pay for the estimated costs of a regular vaginal delivery and a two night stay, for a maximum set amount and the hospital cannot charge you more than that amount. We paid $7,900 and actually received a refund of $1,500 because we were not allowed to stay in our room after the first night.
You can also negotiate a “global fee” with your ob/gyn which we did, which was around $4,500. It covers the cost of the doctor for office visits and delivery but you still have to pay for the ultrasounds and any other tests (e.g. amnio) required during the pregnancy.
We had also obtained a “catastrophic insurance policy” once Lisa was pregnant, which would have covered the cost of any pregnancy related emergencies, including an emergency C-Section (but not a voluntary one). My husband and I ended up paying for a second amnio because we induced labor at 37 weeks and any induction prior to 38 weeks requires an amnio to make sure that the lungs are fully developed. So we had an amnio at around 16 weeks to detect likely birth or other genetic defects, and another at 37 weeks to ensure lung development so that we could induce labor. We didn’t induce delivery for medical reasons. We induced because Lisa lived in the mountains at the time, and we were having a particularly nasty winter that year with a lot of snow where she lived. If Lisa went into labor on the mountain and could not get to Los Angeles, we would have delivered our baby with a doctor neither we nor Lisa knew, at a hospital that had no paperwork on file from us about the surrogacy (therefore no legal right to bring our daughter home that they would be aware of) and with which we didn’t have a financial arrangement (so we would have been billed the full “cash patient” amount). Not to mention, if my husband and I couldn’t get up the mountain to be with Lisa because of the weather, we would have missed the birth of our daughter.
Needless to say, in the grand scheme of things, none of these hurdles mattered anymore. We had a healthy baby girl and were parents. Now the real work began…
Please feel free to share your own experiences below.